
CASH-strapped doctors are threatening to stop visiting sick, elderly residents in nursing homes, citing poor Medicare fees and a lack of trained nurses.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
The Australian Medical Association is warning of a crisis in aged care as doctors increasingly abandon visits to nursing home patients.
A recent AMA Aged Care Survey of more than 600 GPs, consultant physicians and palliative care and geriatrician specialists found that fewer doctors are making visits to residential aged care facilities, but those that do are making more visits and are spending more time with patients.
However, more than 35 per cent of doctors surveyed reported that they plan to not take on new patients and to reduce the number of visits, or stop completely, over the next two years.
Doctors are also concerned at the trend to replace registered and enrolled nurses with personal care attendants, who are not appropriately trained to deal with the health issues older people face.
Many doctors reported that there was sometimes no nurse available for doctors to carry out a clinical handover, and no nurse available to administer medicines after hours.
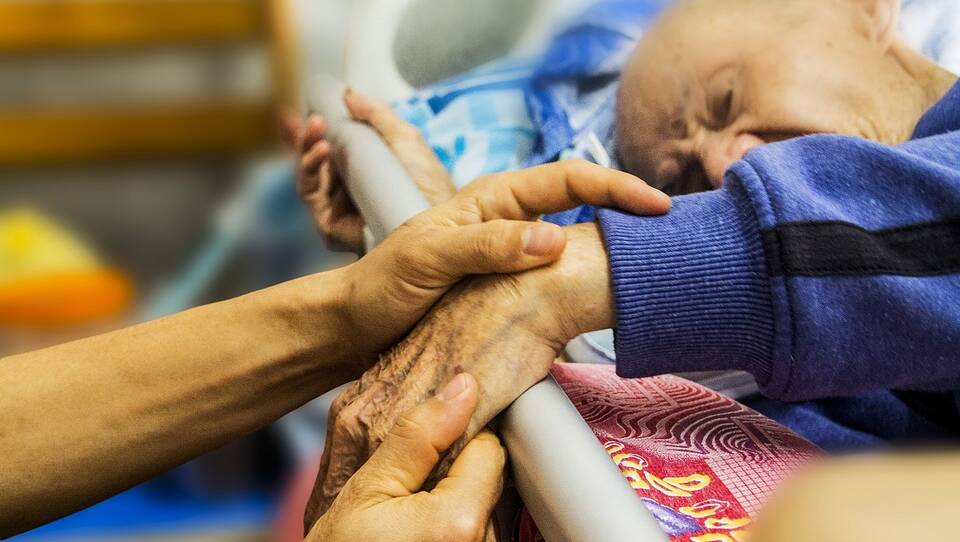
AMA president Tony Bartone, a GP who also makes residential aged care visits in Melbourne, said that the survey raised worrying concerns about the issues involved in providing medical care to older people.
“We are making this report public because now, more than ever, we need action in aged care,” Dr Bartone said.
“Australia is facing an ageing population, with more chronic, complex medical conditions than ever before. The current aged care workforce does not have the capability, capacity and connectedness to adequately meet the needs of older people.
“People living in residential aged care facilities must have timely access to medical practitioners to avoid adverse health events, unnecessary hospitalisations, and associated costs to the health system.”
Dr Bartone said the AMA members surveyed said that having sufficient numbers of experienced nurses available is their top priority, with two-thirds (65.92 per cent) rating this as urgent or extremely urgent.
“Almost 85 per cent said that a nurse, with most specifying a registered nurse, is the level of expertise required to conduct a professionally responsible handover for their patient’s care,” he said.
“This poses serious risks to the health of patients.
“The survey also found that doctors must be adequately compensated for spending time away from their surgery, with 57 per cent rating this as urgent or extremely urgent.
“More than four in five doctors who had decreased their visits to to residential aged care facilities over the past five years said that increasing, unpaid non-contact time was the reason for their decision.
“Fewer than 10 per cent of respondents said that the Medicare Benefits Schedule rebate for visiting patients in aged care facilities was adequate enough to compensate for non-contact time, including locating the patient, filling in scripts and paperwork, talking to relatives, renewing scripts over the telephone, and telephone calls to staff while in their surgery.
“When the GP Aged Care Access Incentive payment ends in April next year, more GPs may abandon visiting aged care facilities.”
Dr Bartone said adequate funding to ensure older people have access to quality medical care through a quality aged care workforce must be a priority.
Leading Age Services Australia, a national peak body for providers of age services across residential care, home care and retirement living described the report as “a cause for concern”.
“A priority for older Australians living in the community or an aged care home is having access to quality and responsive GP care, as many have complex and chronic conditions,” said chief executive Sean Rooney.
He said it was vital that system settings were appropriate to ensure GP care was available for older people whether in their homes or in aged care facilities.
However, he said providing appropriate levels of care was not as simple as the number of staff on duty, or arbitrary staffing ratios.
“Providers design their staffing models to deliver on the most stringent national standards set by the federal government and enforced by the Australian Aged Care Quality Agency,” Mr Rooney said.
“The basis for deciding on staffing levels and their skills mix needs to be driven by the actual care needs of individual residents.”

Pat Sparrow, chief executive of Aged and Community Services Australia which represents not-for-profit accommodation and care services, said it was important all older people had access to health services when needed in a timely manner, regardless of where they lived.
"Doctors have a responsibility to ensure positive health outcomes for older persons living in residential aged care, just as for any other patient they treat,” Ms Sparrow said.
"Aged care providers provide essential care and support for older Australians, many with chronic health conditions, but are not funded to provide hospital-level care.
“Residential aged care is funded at about $260 per resident per day compared to $1900 per patient per day for hospital care.”
Ms Sparrow said providers were increasingly under financial strain with recent data from StewartBrown showing that 41 per cent of residential aged care facilities were making a loss at December 2017 compared with 31 per cent in 2015-16 – and the situation is predicted to get even worse.
“With consumers’ expectations of aged care increasing, and funding pressures continuing to bite, it is time for doctors to recognise aged care facilities do their best to provide quality care with limited resources,” she said.
“Australia can only develop the services frail older Australian want and need now, and into the future, by ensuring we have a well-funded and sustainable residential aged care sector."


