
The corridors of the hospital are filled with an ominous sense of apprehension.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
The tables and chairs from the cafeteria are gone, and there are fewer visitors.
It looks different. Feels different.
Entire departments have been rearranged and re-purposed - ready to accommodate a surge in patients.
And the staff - the doctors, nurses, orderlies, cleaners, support staff and admin - are all waiting. They are watching the news roll in from Italy, Spain and the UK, and seeing the enormous pressure coronavirus is putting on those hospitals and their medical teams.
And they are waiting.
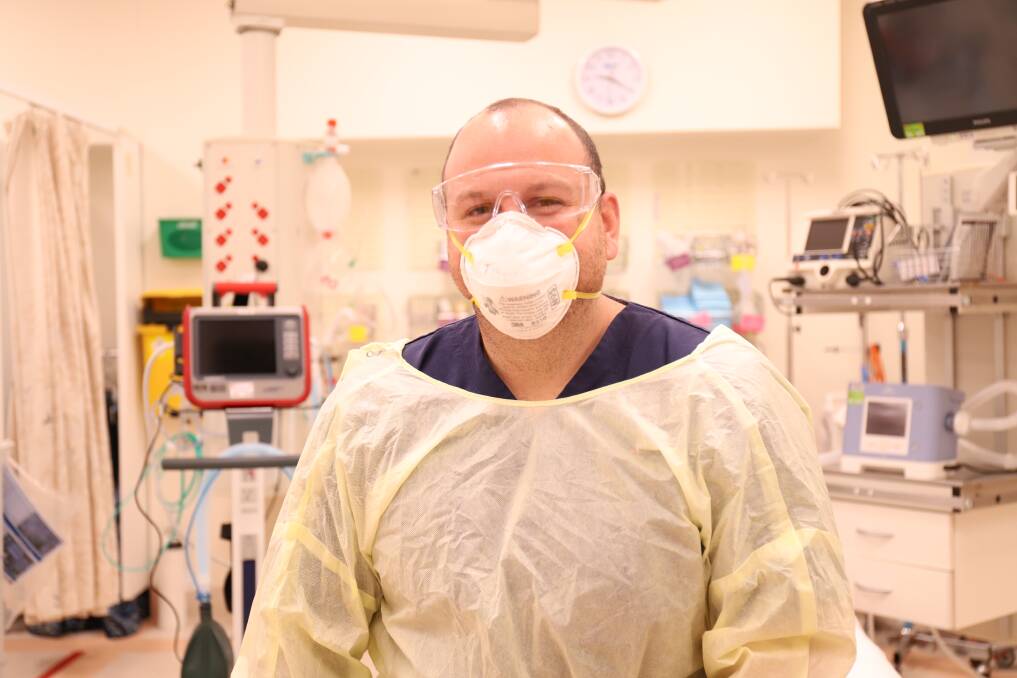
Three weeks ago, Jeremy Pallas - a nurse educator in the emergency department at John Hunter Hospital in Newcastle - was setting up a screening clinic for COVID-19 at the hospital's main entrance.
The staff there had been "working furiously" to prepare for what might be ahead as confirmed cases of COVID-19 continued to climb in Australia.
"Being slightly behind some of the places that are being impacted by the virus - like Italy and the UK and a lot of European countries - and knowing what might be ahead of us gives us a golden opportunity for preparation," Mr Pallas said.

"We can see what's happening around the world, and we know the different ways that this looks like it could go. So there is just this feeling of waiting, and using the time we have left to prepare as much as we possibly can. Lots of the wards are being prepared in different ways, being re-purposed to give us the best capacity we possibly can to accommodate the potential patients that will arrive with this disease."
Mr Pallas said there were "a lot of different feelings" in the hospital.
"But among a lot of my colleagues there is this real sense that people are really linking arms together and getting ready for this challenge," he said.

"It is bigger than the challenges we would normally face, but the preparation is the same, and the team work is the same, and the camaraderie is the same, and we will embrace this challenge in the same way."
He and his colleagues had been pulling some big days.
They shared the same anxieties and concerns about the virus as anyone, but they were used to working calmly under pressure. The waiting was the worst part.
"In the ED, there is an almost ominous feeling," he said. "Everybody is waiting, and while we are waiting, we are listening to reports from our colleagues overseas.
"Once we start seeing patients, that is the thing that is much more familiar to us in the emergency department.
"We are used to seeing 250-plus patients a day. At the moment we are seeing less, and I think that contributes to that feeling of waiting for something to happen.
"But the way we distract ourselves from the nerves is by busying ourselves with other things - like getting the place ready, and getting as much training in as we can."

They were also planning how to welcome and accommodate more medical staff who would be working alongside them should COVID-19 escalate.
Mr Pallas said people in the community were understandably worried.
"I haven't spoken to anyone in the past few weeks who hasn't been a bit panicked and anxious," he said.
But through the screening clinic, the nurses had an opportunity to talk to people about their fears, and offer some reassurance.
His medical colleagues had all gone into these roles knowing they might face some big challenges.
"Every day we come to work knowing there is the potential that one disaster or another will occur," he said. "We know that, and we are ready to take it on everyday. This is a challenge that will be ongoing for a long time. Right now, for the next few months, it is our time to use our tools to make a difference. But there are also people facing things everyday now that they never would have predicted before this.
"People whose jobs aren't there when they go to work in the morning. People who can't take their kids to the park, or do the things they like to do.
"Sure our challenge is a big challenge, and it will be a hard time that we will get through together. But in the scheme of things, it's a challenge we will be prepared for, and it is our part to play in the community."
Outside the hospital environment - in general practice - nurses, doctors, and support staff have been working hard to keep people out of the hospital, and stay safe themselves.
All staff were focused on trying to stay well.
"No one wants us to not get sick more than we do," Mr Pallas laughed.
"We've got the right personal protective equipment (PPE), we have the right training, departments are being totally overhauled to ensure that not only our teams - but the patients that come through - are as safe as they can be.
"It is important for us to take every measure we can to ensure our staff don't get sick. Without them, the building doesn't function the way it is intended to.
"But for the community that rely on this hospital, the most important message is that we are here with them, and this is a challenge we will all face together, and when you need us, we'll be here."

Elizabeth Grist had just come out of a meeting with a room full of Hunter nurses, and the executive director of clinical services in nursing and midwifery was in awe.
The nurses were upskilling. They had worked in intensive care previously, but they wanted a "refresher" in case they were called on to help in a surge.
"But you know what, they are so calm, so professional, they are just wanting to protect their community and do their job," Ms Grist said.
"The staff are amazing. They really are. I am humbled by them. This is an unknown territory. No one could have foreseen this, it just came out of the blue really, when it hit China. It has been absolutely terrifying to see some of those scenes over in Italy and Spain.
"We know what to prepare for, and hopefully it won't come to that here, but we have to prepare."
Ms Grist is also the Health Services Functional Area commander who coordinates disasters.
"I never thought, in my lifetime, I would have to do one like this," she said.
"I've had lots of training over the years. When it was SARS we had prepared, but it never got to this."
Their team initially received criticism when they introduced reduced visiting hours at Hunter New England's 39 hospitals. But as cases of the disease progressed, and the public health messages became louder, there was less push back.

"There was some backlash initially, but I think people are starting to get it now - that our staff are our front line, and we need to protect them," she said.
"If our staff get sick, who have we got to look after the community? Women are still having babies, people are still having other health problems. People are still coming in to casualty with broken legs. That is why it is so important that our staff are protected and able to do their job."
Both retired nurses and undergraduates had been putting their hands up to help in some way.
On Monday, they had advertised for undergraduate nurses and midwives to work alongside experienced staff. By Thursday, they'd had more than 230 applications.
"I haven't had the sense that people are running away from it," Ms Grist said.
"But there is a real hope that we will flatten the curve, and that it won't hit us as hard."
Ms Grist said it was a lot to ask of nurses, and other medical staff, to put themselves and their families at risk.
"They are worried about their families more than anything else," she said.
"We are putting a lot of measures in place. People are getting changed before they go. And if they wear the right protective equipment, people should be fine.
"A lot of education has gone into making sure every single staff member knows how to use their personal protective equipment, and are looking after their own health."
Ms Grist said these heroes were right on the frontline, putting themselves forward to deal with the most critical situations.
"They are prepared to face this challenge, they really are," she said.
"It is a big thing. But this is our job, and this is what we do.
"The message that has come through - loud and clear from them - is that they are here to look after their community as they always do.
"I think we are all scared - all the doctors, nurses, health professionals and people working in the hospital - we are all scared. But we all know we have our job to do.
"I am in total admiration."
Ms Grist wanted to thank all of the hospital staff. Not just the nurses and doctors, but all of the allied health staff, the admin and support staff, the orderlies and cleaners. All of the people who kept the hospital running.
"I have been a nurse for 43 years, and I have never seen such a cohesive response to such a difficult situation," she said.
"They are amazing people. And we all need to thank them. The irony of it is that it is the international year of the nurse and midwife."
Ms Grist said they had planned a big celebration for May 12, in honour of the bicentenary of the birth of the founder of modern nursing, Florence Nightingale. But that had been cancelled.
"This is what we have got instead," she said.

They are the calm and clear and reassuring voices on the end of a phone call, delivering the news when you test positive for COVID-19, or someone you have been in close contact with has.
Rachel Latta is part of a rapidly growing team of contact tracers - nurses, doctors and epidemiologists - for Hunter New England Health.
They are the ones charged with tracking down COVID-19 cases, gleaning vital information about where those people have been, what they have done, and who they have been in close or casual contact with.
Then they find and interview those close contacts - anyone they have spent time with in a confined space, and anyone they have spoken to face-to-face - in the two-to-three weeks prior.
They explain what people need to do next, and why it is so important.
"It's a phone call that sometimes instantly instills fear in people," Ms Latta said.
"People get very nervous, and can sometimes be worried when we phone them, but throughout the conversation we provide some calm and reassurance, and by the end of the call, they often feel more educated and empowered because they know what to do to in order to protect others."
Their work helps population health understand how people are getting coronavirus, and where they are picking it up to track how it is spreading.
"If someone has had close contact, we ask them to self isolate for up to two weeks since their last contact with that person. And that is really important, because that is going to help stop the transmission of coronavirus," she said. "We ask them to stay at home and limit their contact with people outside their household, and ask them to limit - as much as possible - their contact within the household too, so that if they develop symptoms, the number people they have been in contact with is really small. We are trying to stop the spread before it happens."
If you're looking to stay up to date on COVID-19, sign up for our twice-daily digest here.

